Francine Halberg, M.D., is a busy woman. In addition to participating in state and national boards, studies and committees — including her involvement as a steering committee member of the Marin County Women’s Study (marinwomensstudy.org), a project undertaken to determine why breast cancer risk factors do not affect all women in the same way — Halberg is a radiation oncologist at Marin Cancer Institute, where the majority of her own patients are in treatment for breast cancer. Halberg, who graduated medical school from Cornell University and completed an Internship at Stanford University Hospital, has practiced radiation oncology at Marin General Hospital since 1991; the institute was formed in 1992. This year, the Commission on Cancer Accreditation Program of the American College of Surgeons awarded the institute (located adjacent to the hospital in Greenbrae) eight out of eight possible commendations, and cancer survival rates at the hospital surpass the national average — results that reflect the innovative, holistic approach and pioneering techniques of Halberg and her colleagues.
What is the relationship between the Marin Cancer Institute and Marin General Hospital? Marin Cancer Institute is a flagship program of Marin General Hospital — an integral part of the hospital’s mission to serve the residents of Marin. The institute offers a full array of medical and radiation oncologists, surgeons, urologists and breast specialists who provide cancer care in Marin. We collaborate to continuously improve and seamlessly integrate inpatient and outpatient cancer care. We provide services at both ends of the spectrum, from community and physician education and prevention to helping people through the challenges that may face them after treatment.
On average, how many patients does the institute treat in a year — and how does that break down by types of cancer? We currently treat about 700 new cases and follow close to 15,000 patients whom we’ve treated in the past. The most common cancers treated are breast cancer (24 percent of patients), prostate cancer (21 percent) and lung cancer (10 percent). Colorectal and non-prostate urologic cancers each make up about 7 percent of the total. We treat many other types of cancer as well.
What are the average demographics of the breast cancer patients you see at the institute? We have patients in their 20s and all the way up to their 90s. Breast cancer disproportionately affects well-educated Caucasian women, although we certainly see women of all races and ethnic backgrounds at Marin Cancer Institute. The message is that breast cancer is often diagnosed in women with no known risk factors; it can hit anyone. Because our county has so many women diagnosed with breast cancer, we have put together a truly exceptional program to provide the very best possible care. Part of that includes participating in research to determine what causes breast cancer. Marin General Hospital, the County of Marin, Zero Breast Cancer and others are committed to finding out why so many women with excellent access to health care and prevention still have a higher level of risk.
The initial results from the Marin Women’s Study (MWS) add weight to other statewide and national investigations showing that when women stopped taking estrogen and progestin therapy, striking reductions in breast cancer incidence followed. How was the Marin Cancer Institute involved in this study? And what are your thoughts on it? Marin General Hospital has played a key role in the study — with our patients having the highest participation rate of any group — and the importance of the results can’t be over-emphasized. Our investigation of hormone replacement therapy (HRT) and breast cancer was one of the numerous analyses that will eventually come out of the MWS. The fact that our HRT utilization patterns and breast cancer rates both decreased in the time following the Women’s Health Initiative (WHI) gave us some great clues about why overall breast cancer rates declined.
One thing we have learned, however, is that eliminating HRT alone will not stop breast cancer. We need to continue to raise awareness of other factors that increase risk. For example, alcohol consumption: It appears that consumption of more than 4 to 6 drinks per week begins to significantly increase your risk. Additionally, we’re learning that excessive alcohol consumption as a teenager may lead to higher lifelong risk. And there’s a relationship between being overweight and higher breast cancer risk — especially if the weight gain takes place later in life. There also appears to be a strong correlation between risk and not getting enough exercise. We are not out of the woods yet, and Marin Cancer Institute will continue to promote research and education about risk reduction.
What education programs does Marin General Hospital and the Marin Cancer Institute have about breast cancer? There will be a wide array of community education events during Breast Cancer Awareness Month, including our annual breast forum. Look for registration information on our website, marincancerinstitute.org.
You’ve been a radiation oncologist for 20 years. How has the treatment of breast cancer changed in that time? And how has your own approach to and thinking about the disease changed? Our patients are amazing, and their courage and strength inspires us daily. Throughout my career we have kept making progress: Cure rates are up, and patients experience fewer side effects. Cancer treatment today is a team effort with the patient and all of the involved physicians. Each patient is presented to a multidisciplinary tumor board, so she gets a built-in second opinion. By having all the physicians involved in breast cancer work so closely together, we can push our program to be even better. We also review open research studies for each patient — both the initial findings and whether our patients might benefit from participation.
The biggest change I’ve seen during my career is the realization that breast cancer isn’t a single disease — it is many different diseases that we can now define. Understanding that has allowed us to begin to tailor treatment to each individual patient and her specific tumor situation, with improved effectiveness.
The variety of options for patients is greater than ever. Often this allows us to do less than we might have in the past, whether it is a breast-conserving approach, less radiation, avoiding removal of lymph nodes or avoiding chemotherapy when possible. If a mastectomy is chosen, we now have skin and nipple-sparing surgery and a gifted team that makes the latest reconstruction techniques available. We’re now applying personalized medicine — including individual genetic traits — to decide how best to tackle each person’s case.
Because clinical trials have driven tremendous advances in cancer prevention, diagnosis and treatment, we have been participating in them since the late 1970s. Since 1990, we have enrolled 1,346 patients in various trials, approximately 64 patients a year. We have participated in 56 breast cancer trials aimed at prolonging life-effecting cures. Scores more have been done to study drugs that relieve or prevent the symptoms and side effects of the illness and the treatments we use. You don’t have to go to an academic medical center — or even cross a bridge — to have access to the latest research.
Of course, improved technology also is driving improved outcomes, and we have invested to provide the most advanced technology to our patients, from digital mammography to radiation therapy CT simulators, state-of-the-art linear accelerators, 3D-CRT, IMRT, IGRT, Respiratory Gating and stereotactic radiosurgery. Our community has been very generous in helping us acquire this technology, and we are incredibly grateful.
We take tremendous pride in having the highest possible levels of certification. Just this past week, our oncology physicians obtained QOPI Certification. QOPI, the Quality Oncology Practice Initiative of the American Society of Clinical Oncology, is a national certification designed to promote excellence in cancer care by helping practices create a culture of self-examination and improvement — and fewer than 100 practices across the country have been so certified, including six in California. Several health plans recognize it and reward practices for participation.
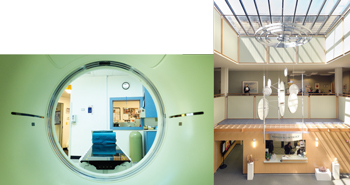 Marin Cancer Institute has pioneered techniques in radiation oncology, one of them being synchronizing the treatment with the breath. Please explain how this is done and what the benefits are. Were you involved in the development of this technique? We are very proud of the fact that our department has pioneered important advances in breast cancer radiation therapy, like this one. We were involved in the development of intensity modulated radiation therapy (IMRT) to improve the ability to deliver very uniform radiation therapy to the breast, minimizing side effects. More recently we helped develop respiratory gating. The idea is that a deep breath moves the patient’s breast up and away from the patient’s heart, making breast radiation therapy even safer for our patients.
Marin Cancer Institute has pioneered techniques in radiation oncology, one of them being synchronizing the treatment with the breath. Please explain how this is done and what the benefits are. Were you involved in the development of this technique? We are very proud of the fact that our department has pioneered important advances in breast cancer radiation therapy, like this one. We were involved in the development of intensity modulated radiation therapy (IMRT) to improve the ability to deliver very uniform radiation therapy to the breast, minimizing side effects. More recently we helped develop respiratory gating. The idea is that a deep breath moves the patient’s breast up and away from the patient’s heart, making breast radiation therapy even safer for our patients.
Currently there is a debate about how often and at what age women should receive mammograms. Your thoughts on this issue? We have a superb and highly regarded breast imaging program headed by Dr. Vida Campbell. She recommends that all women begin annual screening mammography at the age of 40 and notes that the most controversial part of these recommendations seems to be for younger women in their 40s. These young women get some of the most aggressive cancers that we see. It is critical for them to be screened each year in order for us to have the best chance of finding their cancers early. The largest breast cancer trial to date, published in the journal Cancer in February of this year, addressed the efficacy of screening mammography for women between the ages of 40 to 49. This study involved a million women over 16 years and it found a reduction of breast cancer deaths by 29 percent.
Many cancer programs now emphasize a more holistic approach that goes beyond traditional medical treatments of surgery, radiation and chemotherapy. How has the protocol of care for breast cancer changed? We absolutely believe that you cannot just treat cancer — you must treat the whole individual. Patient-centered care involves not just providing the best medical care but also, and very importantly, being attuned to each patient’s emotional and psychosocial needs. When patients are called in for diagnostic testing, they are introduced to a nurse navigator who serves as their advocate and explains their treatment options. The navigator provides education and support throughout the treatment process.
We offer our patients a full spectrum of support services and educational resources through the Marin General Hospital Cancer Resource & Recovery Center and Center for Integrative Health & Wellness, designed to help them heal and continue living with hope. We make sure our patients never feel they are alone and that their entire care team is always there for them.
Marin Cancer Institute’s palliative care specialists also work as an integral part of each patient’s team of caregivers — which includes doctors, nurses, registered dietitians, pharmacists and social workers — to improve and maintain our patients’ quality of life. Palliative care begins at diagnosis and continues during cancer treatment and beyond, helping to address the emotional, physical, practical and spiritual issues of cancer. Family members may also receive palliative care.
Are there lifestyle changes women can make to help prevent breast cancer, or that can help ease treatment during recovery? If I were advising my own daughter, here’s what I would say: Exercise at least four hours a week. We have clinical results that show this significantly reduces breast cancer risk. Reduce or maintain your weight at a healthy level. This is especially important as women get older but applies at all ages. Limit your alcohol intake to less than six glasses per week. Don’t smoke. Just don’t. Even though we are still accumulating all of the data, avoid drinking water from plastic bottles, and limit exposures to phthalates, parabens and other hormone-disrupting compounds such as pesticides in food, cosmetics and home products. Eat lots of vegetables and fruit. No hormone replacement therapy (HRT) if possible. Finally, be a strong advocate for continued research and improved care. There’s so much more to be done.


